18 results
Assessment of endotracheal aspirate culture appropriateness among adult ICU patients at an academic medical center
- Michael Chambers, Romney Humphries, Bryan Harris, Tom Talbot
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, p. s63
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Ventilator-associated pneumonia (VAP) is a significant cause of mortality in intensive care units (ICUs), but minimal research exists regarding the appropriateness of ordering endotracheal aspirate cultures (EACs). We evaluated the diagnostic utility of rationales given for EAC collection in ICUs at an academic medical center to assess potentially inappropriate EAC ordering. Methods: The study population comprised all adult patients admitted to an ICU in 2019 who underwent EAC collection. A random 10% sample from this population, stratified by ICU type, was selected. Clinical and diagnostic characteristics within 24 hours of EAC collection were identified by chart review. Clinical documentation was reviewed to identify ICU provider rationales for ordering EAC. Results: In total, 749 patients underwent EAC collection. Among them, 75 patients comprised the random sample, of whom 7 (9.3%) were excluded due to extubation before culture collection. Figure 1 shows patient distribution by ICU type. From these 68 patients, 105 EACs were collected. Of these, 41 (39%) were positive for potential pathogens, and 59 (56.2%) had explicit rationales for EAC collection, including fever (44.1%), hypoxia (18.6%), leukocytosis (16.9%), secretions (11.9%), shock (10.2%), and radiologic findings (8.5%). Also, 43.8% of EACs had no explicit rationale for collection. Table 1 shows sensitivities, specificities, positive likelihood ratios (LRs), and negative LRs for these rationales and related characteristics. Conclusions: EACs were commonly ordered without clear clinical indications. Of the noted rationales for EAC collections, most performed poorly at predicting positive cultures, which challenged common rationales for ordering EAC. This study could serve as a foundation for diagnostic stewardship interventions for EAC, potentially decreasing unnecessary cultures.
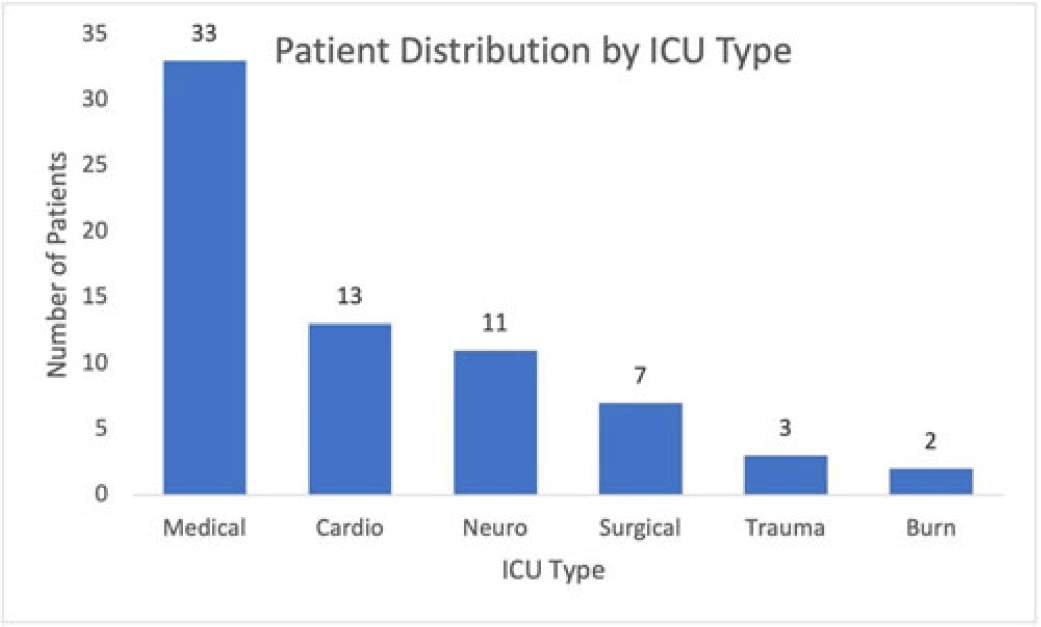
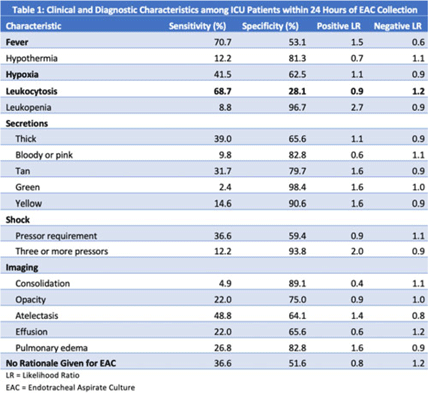
Disclosures: None
Traditional definition of healthcare-associated influenza underestimates cases associated with other healthcare exposures in a population-based surveillance system
- Erin B. Gettler, H. Keipp Talbot, Yuwei Zhu, Danielle Ndi, Edward Mitchel, Tiffanie M. Markus, William Schaffner, Bryan Harris, Thomas R. Talbot
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 11 / November 2023
- Published online by Cambridge University Press:
- 19 April 2023, pp. 1816-1822
- Print publication:
- November 2023
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Objective:
To provide comprehensive population-level estimates of the burden of healthcare-associated influenza.
Design:Retrospective cross-sectional study.
Setting:US Influenza Hospitalization Surveillance Network (FluSurv-NET) during 2012–2013 through 2018–2019 influenza seasons.
Patients:Laboratory-confirmed influenza-related hospitalizations in an 8-county catchment area in Tennessee.
Methods:The incidence of healthcare-associated influenza was determined using the traditional definition (ie, positive influenza test after hospital day 3) in addition to often underrecognized cases associated with recent post-acute care facility admission or a recent acute care hospitalization for a noninfluenza illness in the preceding 7 days.
Results:Among the 5,904 laboratory-confirmed influenza-related hospitalizations, 147 (2.5%) had traditionally defined healthcare-associated influenza. When we included patients with a positive influenza test obtained in the first 3 days of hospitalization and who were either transferred to the hospital directly from a post-acute care facility or who were recently discharged from an acute care facility for a noninfluenza illness in the preceding 7 days, we identified an additional 1,031 cases (17.5% of all influenza-related hospitalizations).
Conclusions:Including influenza cases associated with preadmission healthcare exposures with traditionally defined cases resulted in an 8-fold higher incidence of healthcare-associated influenza. These results emphasize the importance of capturing other healthcare exposures that may serve as the initial site of viral transmission to provide more comprehensive estimates of the burden of healthcare-associated influenza and to inform improved infection prevention strategies.
Universal admission laboratory screening for severe acute respiratory coronavirus virus 2 (SARS-CoV-2) asymptomatic infection across a large health system
- Jennifer L. Cihlar, Bryan D. Harris, Patty W. Wright, Romney M. Humphries, Caroline K. Taylor, Brandi R. Cherry, Thomas R. Talbot
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 1 / January 2023
- Published online by Cambridge University Press:
- 19 December 2022, pp. 68-74
- Print publication:
- January 2023
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background:
Admission laboratory screening for asymptomatic coronavirus disease 2019 (COVID-19) has been utilized to mitigate healthcare-associated severe acute respiratory coronavirus virus 2 (SARS-CoV-2) transmission. An understanding of the impact of such testing across a variety of patient populations is needed.
Methods:SARS-CoV-2 nucleic acid amplification admission testing results for all asymptomatic patients across 4 distinct inpatient facilities between April 20, 2020, and June 14, 2021, were analyzed. Positivity rates and the number needed to test (NNT) to identify 1 asymptomatic infected patient were calculated. Admission results were compared to COVID-19 community incidence rates for the system’s surrounding metropolitan service area. Using a national survey of hospital epidemiologists, a clinically meaningful NNT of 1:100 was identified.
Results:In total, 51,187 tests were collected (positivity rate, 1.8%). During periods of high transmission, the NNT met the clinically relevant threshold in all populations. The NNT approached or met the threshold for most locations during periods of lower transmission. For all transmission levels, the NNT for fully vaccinated patients did not meet the threshold.
Conclusions:Implementing an asymptomatic patient admission testing program can provide clinically relevant data based on the NNT, even during periods of lower transmission and among different patient populations. Limiting admission testing to non–fully vaccinated patients during periods of lower transmission may be a strategy to address resource concerns around this practice. Although the impact of such testing on healthcare-associated COVID-19 among patients and healthcare workers could not be clearly determined, these data provide important information as facilities weigh the costs and benefits of such testing.
Identifying barriers to compliance with a universal inpatient protocol for Staphylococcus aureus nasal decolonization with povidone-iodine
- Rebecca A. Stern, Bryan D. Harris, Mary DeVault, Thomas R. Talbot
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 7 / July 2023
- Published online by Cambridge University Press:
- 26 September 2022, pp. 1167-1170
- Print publication:
- July 2023
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Academic hospital nurses were surveyed to assess adherence barriers to a universal povidone-iodine nasal decolonization protocol to prevent Staphylococcus aureus infection. Low training rates, inadequate supplies, documentation and tracking challenges, patient refusal, and burnout contributed to suboptimal adherence. Prioritizing education is essential but alone is insufficient for successful protocol adoption.
Analysis of Universal admission laboratory screening for SARS-CoV-2 asymptomatic infection across a large health system
- Jennifer Cihlar, Bryan Harris, Patty Wright, Romney Humphries, Kelly (Caroline), Brandi Cherry, Thomas Talbot
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, pp. s10-s11
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Admission laboratory screening for asymptomatic COVID-19 has been utilized to mitigate healthcare-associated SARS-CoV-2 transmission. A better understanding of the impact of such testing across a variety of patient populations is needed. Methods: Beginning April 2020, every patient admitted within an academic healthcare system underwent SARS-CoV-2 PCR testing upon admission. Between April 20, 2020 through June 14, 2021, results were analyzed in asymptomatic patients across 4 inpatient facilities: a tertiary-care adult hospital, a free-standing pediatric hospital, a community-based hospital, and a behavioral health hospital. Positivity rates and the number needed to test (NNT) to identify 1 asymptomatic infected patient were calculated overall, by hospital type, by patient vaccination status, and by CDC-defined levels of community transmission. Weekly community incidence rates of COVID-19 for the system’s metropolitan service area (8 central Tennessee counties) were obtained from Tennessee Department of Health records. Weekly COVID-19 incidence rates per 100,000 people were calculated using US Census Bureau data. Using a national survey of hospital epidemiologists, a clinically meaningful NNT was identified (ie, 1 positive patient per 100 patients tested). A crude admission testing cost (covering testing supplies, reagents, and lab personnel costs) was obtained from operational data ($50 per test) to assess testing utility. Results: In total, 51,187 tests were collected during the study period with a positivity rate of 1.8%. No periods of low transmission were observed (Table 1). During high transmission periods, the NNT met the clinically relevant threshold in all populations. In addition, the NNT approached or met the 1:100 threshold for most locations during periods of less transmission, suggesting continued benefit even as infection rates decline. In all transmission periods, the NNT for non–fully vaccinated patients met the clinically meaningful threshold, in contrast to testing of fully vaccinated patients (Table 2). Discussion: Implementing an asymptomatic patient admission testing program can provide clinically relevant value based on the NNT, even during lower periods of transmission and in different patient populations. Limiting admission testing to non–fully vaccinated patients during periods of lower transmission may be a strategy to address cost and resource concerns around this practice. Further investigations into the impact of booster vaccination and newer SARS-CoV-2 variants on admission testing programs are also necessary. Although the impact of such testing on healthcare-associated COVID-19 among patients and healthcare workers could not be clearly determined, these data provide important information as facilities weigh the costs and benefits of such testing.
Funding: None
Disclosures: None
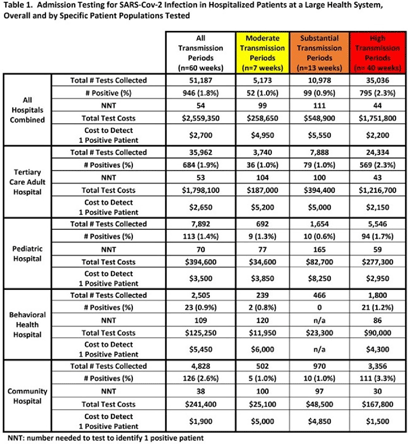
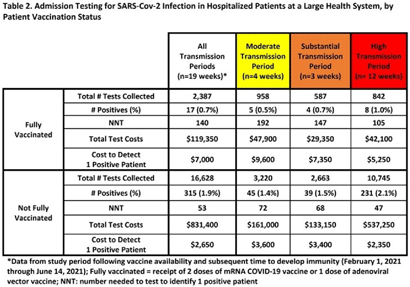
Respiratory Syncytial Virus: An Underrecognized Healthcare-Associated Infection
- Erin Gettler, Thomas Talbot, H. Keipp Talbot, Danielle Ndi, Edward Mitchel, Tiffanie Markus, Bryan Harris, William Schaffner
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue S1 / July 2021
- Published online by Cambridge University Press:
- 29 July 2021, pp. s76-s77
-
- Article
-
- You have access Access
- Open access
- Export citation
-
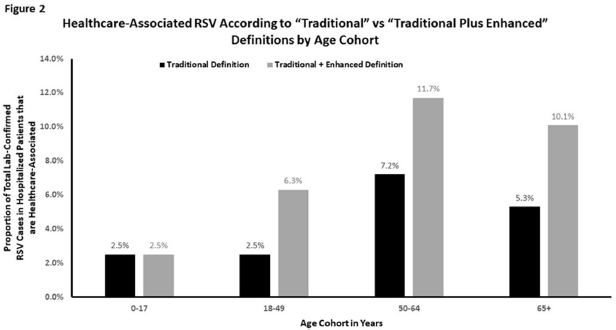
Background: Despite significant morbidity and mortality, estimates of the burden of healthcare-associated viral respiratory infections (HA-VRI) for noninfluenza infections are limited. Of the studies assessing the burden of respiratory syncytial virus (RSV), cases are typically classified as healthcare associated if a positive test result occurred after the first 3 days following admission, which may miss healthcare exposures prior to admission. Utilizing an expanded definition of healthcare-associated RSV, we assessed the estimates of disease prevalence. Methods: This study included laboratory-confirmed cases of RSV in adult and pediatric patients admitted to acute-care hospitals in a catchment area of 8 counties in Tennessee identified between October 1, 2016, and April 30, 2019. Surveillance information was abstracted from hospital and state laboratory databases, hospital infection control databases, reportable condition databases, and electronic health records as a part of the Influenza Hospitalization Surveillance Network by the Emerging Infections Program. Cases were defined as healthcare-associated RSV if laboratory confirmation of infection occurred (1) on or after hospital day 4 (ie, “traditional definition”) or (2) between hospital day 0 and 3 in patients transferred from a chronic care facility or with a recent discharge from another acute-care facility in the 7 days preceding the current index admission (ie, “enhanced definition”). The proportion of laboratory-confirmed RSV designated as HA-VRI using both the traditional definition as well as with the added enhanced definition were compared. Results: We identified 900 cases of RSV in hospitalized patients over the study period. Using the traditional definition for HA-VRI, only 41 (4.6%) were deemed healthcare associated. Adding the cases identified using the enhanced definition, an additional 12 cases (1.3%) were noted in patients transferred from a chronic care facility for the current acute-care admission and 17 cases (1.9%) were noted in patients with a prior acute-care admission in the preceding 7 days. Using our expanded definition, the total proportion of healthcare-associated RSV in this cohort was 69 (7.7%) of 900 compared to 13.1% of cases for influenza (Figure 1). Although the burden of HA-VRI due to RSV was less than that of influenza, when stratified by age, the rate increased to 11.7% for those aged 50–64 years and to 10.1% for those aged ≥65 years (Figure 2). Conclusions: RSV infections are often not included in estimates of HA-VRI, but the proportion of cases that are healthcare associated are substantial. Typical surveillance methods likely underestimate the burden of disease related to RSV, especially for those aged ≥50 years.
Funding: No
Disclosures: None
Figure 1.
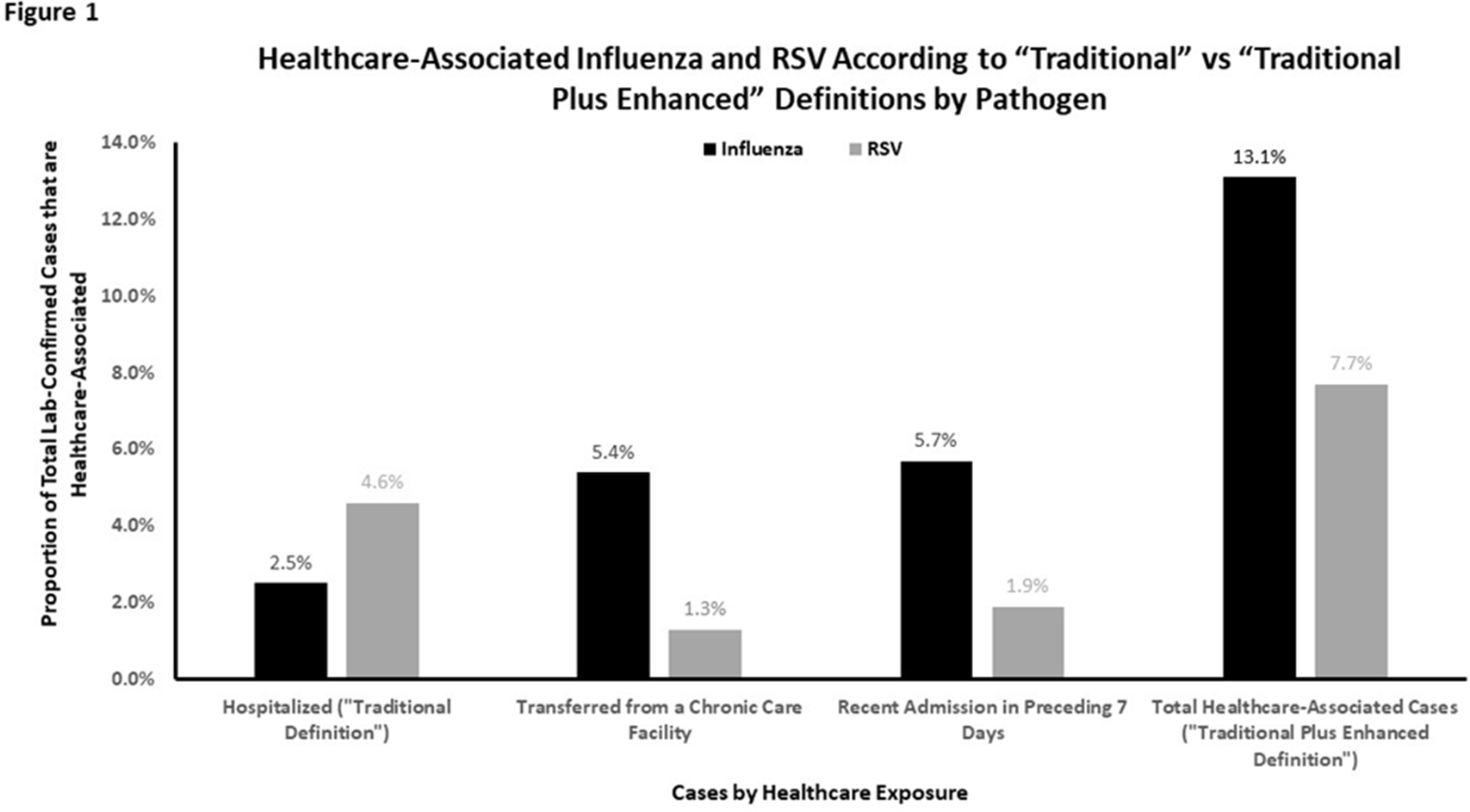
Figure 2.
Traditional Definition of Healthcare-Associated Influenza Underestimates Cases Associated with Other Healthcare Exposures
- Erin Gettler, Thomas Talbot, H. Keipp Talbot, Bryan Harris, Danielle Ndi, Edward Mitchel, Tiffanie Markus, William Schaffner
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue S1 / July 2021
- Published online by Cambridge University Press:
- 29 July 2021, pp. s12-s13
-
- Article
-
- You have access Access
- Open access
- Export citation
-
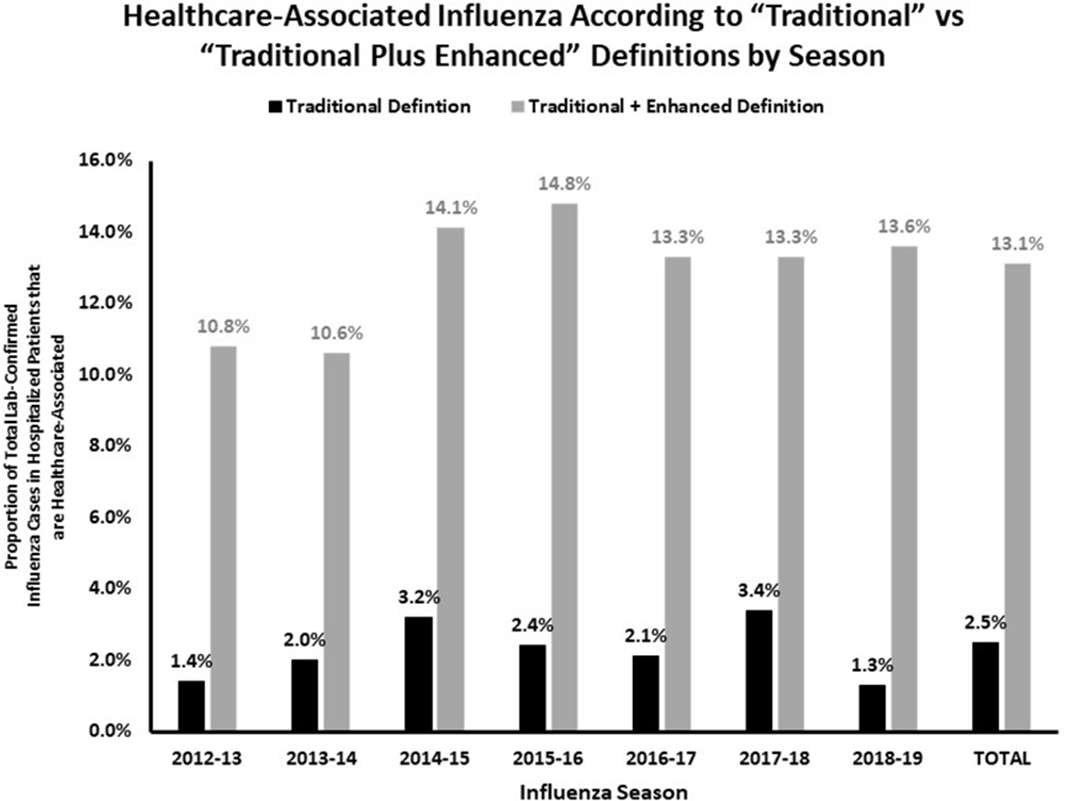
Background: Healthcare-associated transmission of influenza leads to significant morbidity, mortality, and cost. Most studies classify healthcare-associated viral respiratory infections (HA-VRI) as those with a positive test result after the first 3 days following admission, which does not account for healthcare exposures prior to admission. Utilizing an expanded definition of healthcare-associated influenza, we aimed to improve the estimates of disease prevalence on a population level. Methods: This study included laboratory-confirmed cases of influenza in adult and pediatric patients admitted to any acute-care hospital in a catchment area of 8 counties Tennessee identified between October 1, 2012, and April 30, 2019. Surveillance information was abstracted from hospital and state laboratory databases, hospital infection control practitioner databases, reportable condition databases, and electronic health records as a part of the Influenza Hospitalization Surveillance Network (FluSurv-NET) by the Centers for Disease Control and Prevention (CDC) Emerging Infections Program (EIP). Cases were defined as healthcare-associated influenza laboratory confirmation of infection occurred (1) on or after hospital day 4 (“traditional definition”), or (2) between hospital days 0 and 3 in patients transferred from a chronic care facility or with a recent discharge from another acute-care facility in the 7 days preceding the current index admission (ie, enhanced definition). The proportion of laboratory-confirmed influenza designated as HA-VRI using both the traditional definition as well as with the added enhanced definition were compared. Data were imported into Stata software for analysis. Results: We identified 5,904 cases of laboratory-confirmed influenza in hospitalized patients over the study period. Using the traditional definition for HA-VRI, only 147 (2.5%, seasonal range 1.3%–3.4%) were deemed healthcare associated (Figure 1). Adding the cases identified using the enhanced definition, an additional 317 (5.4%, range 2.3%–6.7%) cases were noted in patients transferred from a chronic care facility for the current acute-care admission and 336 cases (5.7%; range, 4.1%–7.4%) were noted in patients with a prior acute-care facility admission in the preceding 7 days. Using our expanded definition, the total proportion of healthcare-associated influenza in this cohort was 772 of 5,904 (13.1%; range, 10.6%–14.8%). Conclusion: HA-VRI due to influenza is an underrecognized infection in hospitalized patients. Limiting surveillance assessment of this important outcome to just those patients with a positive influenza test after hospital day 3 captured only 19% of possible healthcare-associated influenza infections across 7 influenza seasons. These results suggest that the traditionally used definitions of healthcare-associated influenza underestimate the true burden of cases.
Funding: No
Disclosures: None
Figure 1.
Neural predictors and effects of cognitive behavioral therapy for depression: the role of emotional reactivity and regulation – CORRIGENDUM
- Harry Rubin-Falcone, Jochen Weber, Ronit Kishon, Kevin Ochsner, Lauren Delaparte, Bruce Doré, Sudha Raman, Bryan T. Denny, Maria A. Oquendo, J. John Mann, Jeffrey M. Miller
-
- Journal:
- Psychological Medicine / Volume 51 / Issue 12 / September 2021
- Published online by Cambridge University Press:
- 28 July 2021, pp. 2143-2144
-
- Article
-
- You have access Access
- HTML
- Export citation
Assessing coronavirus disease 2019 (COVID-19) transmission to healthcare personnel: The global ACT-HCP case-control study
- Part of
- Robert J. Lentz, Henri Colt, Heidi Chen, Rosa Cordovilla, Spasoje Popevic, Sarabon Tahura, Piero Candoli, Sara Tomassetti, Gerard J. Meachery, Brandon P. Cohen, Bryan D. Harris, Thomas R. Talbot, Fabien Maldonado
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 42 / Issue 4 / April 2021
- Published online by Cambridge University Press:
- 09 September 2020, pp. 381-387
- Print publication:
- April 2021
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Objective:
To characterize associations between exposures within and outside the medical workplace with healthcare personnel (HCP) SARS-CoV-2 infection, including the effect of various forms of respiratory protection.
Design:Case–control study.
Setting:We collected data from international participants via an online survey.
Participants:In total, 1,130 HCP (244 cases with laboratory-confirmed COVID-19, and 886 controls healthy throughout the pandemic) from 67 countries not meeting prespecified exclusion (ie, healthy but not working, missing workplace exposure data, COVID symptoms without lab confirmation) were included in this study.
Methods:Respondents were queried regarding workplace exposures, respiratory protection, and extra-occupational activities. Odds ratios for HCP infection were calculated using multivariable logistic regression and sensitivity analyses controlling for confounders and known biases.
Results:HCP infection was associated with non–aerosol-generating contact with COVID-19 patients (adjusted OR, 1.4; 95% CI, 1.04–1.9; P = .03) and extra-occupational exposures including gatherings of ≥10 people, patronizing restaurants or bars, and public transportation (adjusted OR range, 3.1–16.2). Respirator use during aerosol-generating procedures (AGPs) was associated with lower odds of HCP infection (adjusted OR, 0.4; 95% CI, 0.2–0.8, P = .005), as was exposure to intensive care and dedicated COVID units, negative pressure rooms, and personal protective equipment (PPE) observers (adjusted OR range, 0.4–0.7).
Conclusions:COVID-19 transmission to HCP was associated with medical exposures currently considered lower-risk and multiple extra-occupational exposures, and exposures associated with proper use of appropriate PPE were protective. Closer scrutiny of infection control measures surrounding healthcare activities and medical settings considered lower risk, and continued awareness of the risks of public congregation, may reduce the incidence of HCP infection.
Use of airborne infection isolation in potential cases of pulmonary tuberculosis
- James H. England, Daniel W. Byrne, Bryan D. Harris, Thomas R. Talbot
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue 5 / May 2020
- Published online by Cambridge University Press:
- 16 March 2020, pp. 505-509
- Print publication:
- May 2020
-
- Article
- Export citation
-
Objective:
To identify risk factors of patients placed in airborne infection isolation (AII) for possible pulmonary tuberculosis (TB) to better predict TB diagnosis and allow more judicious use of AII.
Methods:Case-control, retrospective study at a single tertiary-care academic medical center. The study included all adult patients admitted from October 1, 2014, through October 31, 2017, who were placed in AII for possible pulmonary TB. Cases were defined as those ultimately diagnosed with pulmonary TB. Controls were defined as those not diagnosed with pulmonary TB. Those with TB diagnosed prior to admission were excluded. In total, 662 admissions (558 patients) were included.
Results:Overall, 15 cases of pulmonary TB were identified (2.7%); of these, 2 were people living with human immunodeficiency virus (HIV; PLWH). Statistical analysis was limited by low case number. Those diagnosed with pulmonary TB were more likely to have been born outside the United States (53% vs 13%; P < .001) and to have had prior positive TB testing, regardless of prior treatment (50% vs 19%; P = .015). A multivariate analysis using non–US birth and prior positive TB testing predicted an 18.2% probability of pulmonary TB diagnosis when present, compared with 1.0% if both factors were not present.
Conclusions:The low number of pulmonary TB cases indicated AII overuse, especially in PLWH, and more judicious use of AII is warranted. High-risk groups, including those born outside the United States and those with prior positive TB testing, should be considered for AII in the appropriate clinical setting.
Regional to global correlation of Eocene–Oligocene boundary transition successions using biostratigraphic, geophysical and geochemical methods
- Brooks B. Ellwood, Lawrence Febo, Laurie Anderson, Rebecca T. Hackworth, Guy H. Means, Jonathon A. Bryan, Jonathan Tomkin, Harry Rowe, Luigi Jovane
-
- Journal:
- Geological Magazine / Volume 157 / Issue 1 / January 2020
- Published online by Cambridge University Press:
- 12 July 2019, pp. 80-100
-
- Article
-
- You have access Access
- HTML
- Export citation
-
Regional to global high-resolution correlation and timing is critical when attempting to answer important geological questions, such as the greenhouse to icehouse transition that occurred during the Eocene–Oligocene boundary transition. Timing of these events on a global scale can only be answered using correlation among many sections, and multiple correlation proxies, including biostratigraphy, lithostratigraphy, geochemistry and geophysical methods. Here we present litho- and biostratigraphy for five successions located in the southeastern USA. To broaden the scope of correlation, we also employ carbon and oxygen stable isotope and magnetic susceptibility (χ) data to interpret these sections regionally, and correlate to the Global Boundary Stratotype Section and Point (GSSP) near Massignano in central Italy. Our results indicate that approaching the Eocene–Oligocene boundary, climate warmed slightly, but then δ18O data exhibit an abrupt c. +5 ‰ positive shift towards cooling that reached a maximum c. 1 m below the boundary at St Stephens Quarry, Alabama. This shift was accompanied by a c. −3 ‰ negative shift in δ13C interpreted to indicate environmental changes associated with the onset of the Eocene–Oligocene boundary planktonic foraminiferal extinction event. The observed cold pulse may be responsible for the final extinction of Hantkeninidae, used to define the beginning of the Rupelian Stage. Immediately preceding the boundary, Hantkeninidae species dropped significantly in abundance and size (pre-extinction dwarfing occurring before the final Eocene–Oligocene extinctions), and these changes may be the reason for inconsistencies in past Eocene–Oligocene boundary placement in the southeastern USA.
Neural predictors and effects of cognitive behavioral therapy for depression: the role of emotional reactivity and regulation
- Harry Rubin-Falcone, Jochen Weber, Ronit Kishon, Kevin Ochsner, Lauren Delaparte, Bruce Doré, Sudha Raman, Bryan T. Denny, Maria A. Oquendo, J. John Mann, Jeffrey M. Miller
-
- Journal:
- Psychological Medicine / Volume 50 / Issue 1 / January 2020
- Published online by Cambridge University Press:
- 11 February 2019, pp. 146-160
-
- Article
- Export citation
-
Background
Cognitive behavioral therapy (CBT) is an effective treatment for many patients suffering from major depressive disorder (MDD), but predictors of treatment outcome are lacking, and little is known about its neural mechanisms. We recently identified longitudinal changes in neural correlates of conscious emotion regulation that scaled with clinical responses to CBT for MDD, using a negative autobiographical memory-based task.
MethodsWe now examine the neural correlates of emotional reactivity and emotion regulation during viewing of emotionally salient images as predictors of treatment outcome with CBT for MDD, and the relationship between longitudinal change in functional magnetic resonance imaging (fMRI) responses and clinical outcomes. Thirty-two participants with current MDD underwent baseline MRI scanning followed by 14 sessions of CBT. The fMRI task measured emotional reactivity and emotion regulation on separate trials using standardized images from the International Affective Pictures System. Twenty-one participants completed post-treatment scanning. Last observation carried forward was used to estimate clinical outcome for non-completers.
ResultsPre-treatment emotional reactivity Blood Oxygen Level-Dependent (BOLD) signal within hippocampus including CA1 predicted worse treatment outcome. In contrast, better treatment outcome was associated with increased down-regulation of BOLD activity during emotion regulation from time 1 to time 2 in precuneus, occipital cortex, and middle frontal gyrus.
ConclusionsCBT may modulate the neural circuitry of emotion regulation. The neural correlates of emotional reactivity may be more strongly predictive of CBT outcome. The finding that treatment outcome was predicted by BOLD signal in CA1 may suggest overgeneralized memory as a negative prognostic factor in CBT outcome.
Ventilator Bundle Compliance and Risk of Ventilator-Associated Events
- Bryan D. Harris, Gale A. Thomas, Matthew H. Greene, Steven S. Spires, Thomas R. Talbot
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 39 / Issue 6 / June 2018
- Published online by Cambridge University Press:
- 17 May 2018, pp. 637-643
- Print publication:
- June 2018
-
- Article
- Export citation
-
OBJECTIVE
Ventilator bundles encompass practices that reduce the risk of ventilator complications, including ventilator-associated pneumonia. The impact of ventilator bundles on the risk of developing ventilator-associated events (VAEs) is unknown. We sought to determine whether decreased compliance to the ventilator bundle increases the risk for VAE development.
DESIGNNested case-control study.
SETTINGThis study was conducted at 6 adult intensive care units at an academic tertiary-care center in Tennessee.
PATIENTSIn total, 273 patients with VAEs were randomly matched in a 1:4 ratio to controls by mechanical ventilation duration and ICU type.
METHODSControls were selected from the primary study population at risk for a VAE after being mechanically ventilated for the same number of days as a specified case. Using conditional logistic regression analysis, overall cumulative compliance, and compliance with individual components of the bundle in the 3 and 7 days prior to VAE development (or the control match day) were examined.
RESULTSOverall bundle compliance at 3 days (odds ratio [OR], 1.15; P=.34) and 7 days prior to VAE diagnosis (OR, 0.96; P=.83) were not associated with VAE development. This finding did not change when limiting the outcome to infection-related ventilator-associated complications (IVACs) and after adjusting for age and gender. In the examination of compliance with specific bundle components increased compliance with chlorhexidine oral care was associated with increased risk of VAE development in all analyses.
CONCLUSIONSVentilator bundle compliance was not associated with a reduced risk for VAEs. Higher compliance with chlorhexidine oral care was associated with a greater risk for VAE development.
Infect Control Hosp Epidemiol 2018;39:637–643
Contributors
-
- By Mitchell Aboulafia, Frederick Adams, Marilyn McCord Adams, Robert M. Adams, Laird Addis, James W. Allard, David Allison, William P. Alston, Karl Ameriks, C. Anthony Anderson, David Leech Anderson, Lanier Anderson, Roger Ariew, David Armstrong, Denis G. Arnold, E. J. Ashworth, Margaret Atherton, Robin Attfield, Bruce Aune, Edward Wilson Averill, Jody Azzouni, Kent Bach, Andrew Bailey, Lynne Rudder Baker, Thomas R. Baldwin, Jon Barwise, George Bealer, William Bechtel, Lawrence C. Becker, Mark A. Bedau, Ernst Behler, José A. Benardete, Ermanno Bencivenga, Jan Berg, Michael Bergmann, Robert L. Bernasconi, Sven Bernecker, Bernard Berofsky, Rod Bertolet, Charles J. Beyer, Christian Beyer, Joseph Bien, Joseph Bien, Peg Birmingham, Ivan Boh, James Bohman, Daniel Bonevac, Laurence BonJour, William J. Bouwsma, Raymond D. Bradley, Myles Brand, Richard B. Brandt, Michael E. Bratman, Stephen E. Braude, Daniel Breazeale, Angela Breitenbach, Jason Bridges, David O. Brink, Gordon G. Brittan, Justin Broackes, Dan W. Brock, Aaron Bronfman, Jeffrey E. Brower, Bartosz Brozek, Anthony Brueckner, Jeffrey Bub, Lara Buchak, Otavio Bueno, Ann E. Bumpus, Robert W. Burch, John Burgess, Arthur W. Burks, Panayot Butchvarov, Robert E. Butts, Marina Bykova, Patrick Byrne, David Carr, Noël Carroll, Edward S. Casey, Victor Caston, Victor Caston, Albert Casullo, Robert L. Causey, Alan K. L. Chan, Ruth Chang, Deen K. Chatterjee, Andrew Chignell, Roderick M. Chisholm, Kelly J. Clark, E. J. Coffman, Robin Collins, Brian P. Copenhaver, John Corcoran, John Cottingham, Roger Crisp, Frederick J. Crosson, Antonio S. Cua, Phillip D. Cummins, Martin Curd, Adam Cureton, Andrew Cutrofello, Stephen Darwall, Paul Sheldon Davies, Wayne A. Davis, Timothy Joseph Day, Claudio de Almeida, Mario De Caro, Mario De Caro, John Deigh, C. F. Delaney, Daniel C. Dennett, Michael R. DePaul, Michael Detlefsen, Daniel Trent Devereux, Philip E. Devine, John M. Dillon, Martin C. Dillon, Robert DiSalle, Mary Domski, Alan Donagan, Paul Draper, Fred Dretske, Mircea Dumitru, Wilhelm Dupré, Gerald Dworkin, John Earman, Ellery Eells, Catherine Z. Elgin, Berent Enç, Ronald P. Endicott, Edward Erwin, John Etchemendy, C. Stephen Evans, Susan L. Feagin, Solomon Feferman, Richard Feldman, Arthur Fine, Maurice A. Finocchiaro, William FitzPatrick, Richard E. Flathman, Gvozden Flego, Richard Foley, Graeme Forbes, Rainer Forst, Malcolm R. Forster, Daniel Fouke, Patrick Francken, Samuel Freeman, Elizabeth Fricker, Miranda Fricker, Michael Friedman, Michael Fuerstein, Richard A. Fumerton, Alan Gabbey, Pieranna Garavaso, Daniel Garber, Jorge L. A. Garcia, Robert K. Garcia, Don Garrett, Philip Gasper, Gerald Gaus, Berys Gaut, Bernard Gert, Roger F. Gibson, Cody Gilmore, Carl Ginet, Alan H. Goldman, Alvin I. Goldman, Alfonso Gömez-Lobo, Lenn E. Goodman, Robert M. Gordon, Stefan Gosepath, Jorge J. E. Gracia, Daniel W. Graham, George A. Graham, Peter J. Graham, Richard E. Grandy, I. Grattan-Guinness, John Greco, Philip T. Grier, Nicholas Griffin, Nicholas Griffin, David A. Griffiths, Paul J. Griffiths, Stephen R. Grimm, Charles L. Griswold, Charles B. Guignon, Pete A. Y. Gunter, Dimitri Gutas, Gary Gutting, Paul Guyer, Kwame Gyekye, Oscar A. Haac, Raul Hakli, Raul Hakli, Michael Hallett, Edward C. Halper, Jean Hampton, R. James Hankinson, K. R. Hanley, Russell Hardin, Robert M. Harnish, William Harper, David Harrah, Kevin Hart, Ali Hasan, William Hasker, John Haugeland, Roger Hausheer, William Heald, Peter Heath, Richard Heck, John F. Heil, Vincent F. Hendricks, Stephen Hetherington, Francis Heylighen, Kathleen Marie Higgins, Risto Hilpinen, Harold T. Hodes, Joshua Hoffman, Alan Holland, Robert L. Holmes, Richard Holton, Brad W. Hooker, Terence E. Horgan, Tamara Horowitz, Paul Horwich, Vittorio Hösle, Paul Hoβfeld, Daniel Howard-Snyder, Frances Howard-Snyder, Anne Hudson, Deal W. Hudson, Carl A. Huffman, David L. Hull, Patricia Huntington, Thomas Hurka, Paul Hurley, Rosalind Hursthouse, Guillermo Hurtado, Ronald E. Hustwit, Sarah Hutton, Jonathan Jenkins Ichikawa, Harry A. Ide, David Ingram, Philip J. Ivanhoe, Alfred L. Ivry, Frank Jackson, Dale Jacquette, Joseph Jedwab, Richard Jeffrey, David Alan Johnson, Edward Johnson, Mark D. Jordan, Richard Joyce, Hwa Yol Jung, Robert Hillary Kane, Tomis Kapitan, Jacquelyn Ann K. Kegley, James A. Keller, Ralph Kennedy, Sergei Khoruzhii, Jaegwon Kim, Yersu Kim, Nathan L. King, Patricia Kitcher, Peter D. Klein, E. D. Klemke, Virginia Klenk, George L. Kline, Christian Klotz, Simo Knuuttila, Joseph J. Kockelmans, Konstantin Kolenda, Sebastian Tomasz Kołodziejczyk, Isaac Kramnick, Richard Kraut, Fred Kroon, Manfred Kuehn, Steven T. Kuhn, Henry E. Kyburg, John Lachs, Jennifer Lackey, Stephen E. Lahey, Andrea Lavazza, Thomas H. Leahey, Joo Heung Lee, Keith Lehrer, Dorothy Leland, Noah M. Lemos, Ernest LePore, Sarah-Jane Leslie, Isaac Levi, Andrew Levine, Alan E. Lewis, Daniel E. Little, Shu-hsien Liu, Shu-hsien Liu, Alan K. L. Chan, Brian Loar, Lawrence B. Lombard, John Longeway, Dominic McIver Lopes, Michael J. Loux, E. J. Lowe, Steven Luper, Eugene C. Luschei, William G. Lycan, David Lyons, David Macarthur, Danielle Macbeth, Scott MacDonald, Jacob L. Mackey, Louis H. Mackey, Penelope Mackie, Edward H. Madden, Penelope Maddy, G. B. Madison, Bernd Magnus, Pekka Mäkelä, Rudolf A. Makkreel, David Manley, William E. Mann (W.E.M.), Vladimir Marchenkov, Peter Markie, Jean-Pierre Marquis, Ausonio Marras, Mike W. Martin, A. P. Martinich, William L. McBride, David McCabe, Storrs McCall, Hugh J. McCann, Robert N. McCauley, John J. McDermott, Sarah McGrath, Ralph McInerny, Daniel J. McKaughan, Thomas McKay, Michael McKinsey, Brian P. McLaughlin, Ernan McMullin, Anthonie Meijers, Jack W. Meiland, William Jason Melanson, Alfred R. Mele, Joseph R. Mendola, Christopher Menzel, Michael J. Meyer, Christian B. Miller, David W. Miller, Peter Millican, Robert N. Minor, Phillip Mitsis, James A. Montmarquet, Michael S. Moore, Tim Moore, Benjamin Morison, Donald R. Morrison, Stephen J. Morse, Paul K. Moser, Alexander P. D. Mourelatos, Ian Mueller, James Bernard Murphy, Mark C. Murphy, Steven Nadler, Jan Narveson, Alan Nelson, Jerome Neu, Samuel Newlands, Kai Nielsen, Ilkka Niiniluoto, Carlos G. Noreña, Calvin G. Normore, David Fate Norton, Nikolaj Nottelmann, Donald Nute, David S. Oderberg, Steve Odin, Michael O’Rourke, Willard G. Oxtoby, Heinz Paetzold, George S. Pappas, Anthony J. Parel, Lydia Patton, R. P. Peerenboom, Francis Jeffry Pelletier, Adriaan T. Peperzak, Derk Pereboom, Jaroslav Peregrin, Glen Pettigrove, Philip Pettit, Edmund L. Pincoffs, Andrew Pinsent, Robert B. Pippin, Alvin Plantinga, Louis P. Pojman, Richard H. Popkin, John F. Post, Carl J. Posy, William J. Prior, Richard Purtill, Michael Quante, Philip L. Quinn, Philip L. Quinn, Elizabeth S. Radcliffe, Diana Raffman, Gerard Raulet, Stephen L. Read, Andrews Reath, Andrew Reisner, Nicholas Rescher, Henry S. Richardson, Robert C. Richardson, Thomas Ricketts, Wayne D. Riggs, Mark Roberts, Robert C. Roberts, Luke Robinson, Alexander Rosenberg, Gary Rosenkranz, Bernice Glatzer Rosenthal, Adina L. Roskies, William L. Rowe, T. M. Rudavsky, Michael Ruse, Bruce Russell, Lilly-Marlene Russow, Dan Ryder, R. M. Sainsbury, Joseph Salerno, Nathan Salmon, Wesley C. Salmon, Constantine Sandis, David H. Sanford, Marco Santambrogio, David Sapire, Ruth A. Saunders, Geoffrey Sayre-McCord, Charles Sayward, James P. Scanlan, Richard Schacht, Tamar Schapiro, Frederick F. Schmitt, Jerome B. Schneewind, Calvin O. Schrag, Alan D. Schrift, George F. Schumm, Jean-Loup Seban, David N. Sedley, Kenneth Seeskin, Krister Segerberg, Charlene Haddock Seigfried, Dennis M. Senchuk, James F. Sennett, William Lad Sessions, Stewart Shapiro, Tommie Shelby, Donald W. Sherburne, Christopher Shields, Roger A. Shiner, Sydney Shoemaker, Robert K. Shope, Kwong-loi Shun, Wilfried Sieg, A. John Simmons, Robert L. Simon, Marcus G. Singer, Georgette Sinkler, Walter Sinnott-Armstrong, Matti T. Sintonen, Lawrence Sklar, Brian Skyrms, Robert C. Sleigh, Michael Anthony Slote, Hans Sluga, Barry Smith, Michael Smith, Robin Smith, Robert Sokolowski, Robert C. Solomon, Marta Soniewicka, Philip Soper, Ernest Sosa, Nicholas Southwood, Paul Vincent Spade, T. L. S. Sprigge, Eric O. Springsted, George J. Stack, Rebecca Stangl, Jason Stanley, Florian Steinberger, Sören Stenlund, Christopher Stephens, James P. Sterba, Josef Stern, Matthias Steup, M. A. Stewart, Leopold Stubenberg, Edith Dudley Sulla, Frederick Suppe, Jere Paul Surber, David George Sussman, Sigrún Svavarsdóttir, Zeno G. Swijtink, Richard Swinburne, Charles C. Taliaferro, Robert B. Talisse, John Tasioulas, Paul Teller, Larry S. Temkin, Mark Textor, H. S. Thayer, Peter Thielke, Alan Thomas, Amie L. Thomasson, Katherine Thomson-Jones, Joshua C. Thurow, Vzalerie Tiberius, Terrence N. Tice, Paul Tidman, Mark C. Timmons, William Tolhurst, James E. Tomberlin, Rosemarie Tong, Lawrence Torcello, Kelly Trogdon, J. D. Trout, Robert E. Tully, Raimo Tuomela, John Turri, Martin M. Tweedale, Thomas Uebel, Jennifer Uleman, James Van Cleve, Harry van der Linden, Peter van Inwagen, Bryan W. Van Norden, René van Woudenberg, Donald Phillip Verene, Samantha Vice, Thomas Vinci, Donald Wayne Viney, Barbara Von Eckardt, Peter B. M. Vranas, Steven J. Wagner, William J. Wainwright, Paul E. Walker, Robert E. Wall, Craig Walton, Douglas Walton, Eric Watkins, Richard A. Watson, Michael V. Wedin, Rudolph H. Weingartner, Paul Weirich, Paul J. Weithman, Carl Wellman, Howard Wettstein, Samuel C. Wheeler, Stephen A. White, Jennifer Whiting, Edward R. Wierenga, Michael Williams, Fred Wilson, W. Kent Wilson, Kenneth P. Winkler, John F. Wippel, Jan Woleński, Allan B. Wolter, Nicholas P. Wolterstorff, Rega Wood, W. Jay Wood, Paul Woodruff, Alison Wylie, Gideon Yaffe, Takashi Yagisawa, Yutaka Yamamoto, Keith E. Yandell, Xiaomei Yang, Dean Zimmerman, Günter Zoller, Catherine Zuckert, Michael Zuckert, Jack A. Zupko (J.A.Z.)
- Edited by Robert Audi, University of Notre Dame, Indiana
-
- Book:
- The Cambridge Dictionary of Philosophy
- Published online:
- 05 August 2015
- Print publication:
- 27 April 2015, pp ix-xxx
-
- Chapter
- Export citation
List of Contributors
- Edited by Claudia Rapp, Universität Wien, Austria, H. A. Drake, University of California, Santa Barbara
-
- Book:
- The City in the Classical and Post-Classical World
- Published online:
- 05 April 2014
- Print publication:
- 14 April 2014, pp xi-xiv
-
- Chapter
- Export citation
Contributors
-
- By Rose Teteki Abbey, K. C. Abraham, David Tuesday Adamo, LeRoy H. Aden, Efrain Agosto, Victor Aguilan, Gillian T. W. Ahlgren, Charanjit Kaur AjitSingh, Dorothy B E A Akoto, Giuseppe Alberigo, Daniel E. Albrecht, Ruth Albrecht, Daniel O. Aleshire, Urs Altermatt, Anand Amaladass, Michael Amaladoss, James N. Amanze, Lesley G. Anderson, Thomas C. Anderson, Victor Anderson, Hope S. Antone, María Pilar Aquino, Paula Arai, Victorio Araya Guillén, S. Wesley Ariarajah, Ellen T. Armour, Brett Gregory Armstrong, Atsuhiro Asano, Naim Stifan Ateek, Mahmoud Ayoub, John Alembillah Azumah, Mercedes L. García Bachmann, Irena Backus, J. Wayne Baker, Mieke Bal, Lewis V. Baldwin, William Barbieri, António Barbosa da Silva, David Basinger, Bolaji Olukemi Bateye, Oswald Bayer, Daniel H. Bays, Rosalie Beck, Nancy Elizabeth Bedford, Guy-Thomas Bedouelle, Chorbishop Seely Beggiani, Wolfgang Behringer, Christopher M. Bellitto, Byard Bennett, Harold V. Bennett, Teresa Berger, Miguel A. Bernad, Henley Bernard, Alan E. Bernstein, Jon L. Berquist, Johannes Beutler, Ana María Bidegain, Matthew P. Binkewicz, Jennifer Bird, Joseph Blenkinsopp, Dmytro Bondarenko, Paulo Bonfatti, Riet en Pim Bons-Storm, Jessica A. Boon, Marcus J. Borg, Mark Bosco, Peter C. Bouteneff, François Bovon, William D. Bowman, Paul S. Boyer, David Brakke, Richard E. Brantley, Marcus Braybrooke, Ian Breward, Ênio José da Costa Brito, Jewel Spears Brooker, Johannes Brosseder, Nicholas Canfield Read Brown, Robert F. Brown, Pamela K. Brubaker, Walter Brueggemann, Bishop Colin O. Buchanan, Stanley M. Burgess, Amy Nelson Burnett, J. Patout Burns, David B. Burrell, David Buttrick, James P. Byrd, Lavinia Byrne, Gerado Caetano, Marcos Caldas, Alkiviadis Calivas, William J. Callahan, Salvatore Calomino, Euan K. Cameron, William S. Campbell, Marcelo Ayres Camurça, Daniel F. Caner, Paul E. Capetz, Carlos F. Cardoza-Orlandi, Patrick W. Carey, Barbara Carvill, Hal Cauthron, Subhadra Mitra Channa, Mark D. Chapman, James H. Charlesworth, Kenneth R. Chase, Chen Zemin, Luciano Chianeque, Philip Chia Phin Yin, Francisca H. Chimhanda, Daniel Chiquete, John T. Chirban, Soobin Choi, Robert Choquette, Mita Choudhury, Gerald Christianson, John Chryssavgis, Sejong Chun, Esther Chung-Kim, Charles M. A. Clark, Elizabeth A. Clark, Sathianathan Clarke, Fred Cloud, John B. Cobb, W. Owen Cole, John A Coleman, John J. Collins, Sylvia Collins-Mayo, Paul K. Conkin, Beth A. Conklin, Sean Connolly, Demetrios J. Constantelos, Michael A. Conway, Paula M. Cooey, Austin Cooper, Michael L. Cooper-White, Pamela Cooper-White, L. William Countryman, Sérgio Coutinho, Pamela Couture, Shannon Craigo-Snell, James L. Crenshaw, David Crowner, Humberto Horacio Cucchetti, Lawrence S. Cunningham, Elizabeth Mason Currier, Emmanuel Cutrone, Mary L. Daniel, David D. Daniels, Robert Darden, Rolf Darge, Isaiah Dau, Jeffry C. Davis, Jane Dawson, Valentin Dedji, John W. de Gruchy, Paul DeHart, Wendy J. Deichmann Edwards, Miguel A. De La Torre, George E. Demacopoulos, Thomas de Mayo, Leah DeVun, Beatriz de Vasconcellos Dias, Dennis C. Dickerson, John M. Dillon, Luis Miguel Donatello, Igor Dorfmann-Lazarev, Susanna Drake, Jonathan A. Draper, N. Dreher Martin, Otto Dreydoppel, Angelyn Dries, A. J. Droge, Francis X. D'Sa, Marilyn Dunn, Nicole Wilkinson Duran, Rifaat Ebied, Mark J. Edwards, William H. Edwards, Leonard H. Ehrlich, Nancy L. Eiesland, Martin Elbel, J. Harold Ellens, Stephen Ellingson, Marvin M. Ellison, Robert Ellsberg, Jean Bethke Elshtain, Eldon Jay Epp, Peter C. Erb, Tassilo Erhardt, Maria Erling, Noel Leo Erskine, Gillian R. Evans, Virginia Fabella, Michael A. Fahey, Edward Farley, Margaret A. Farley, Wendy Farley, Robert Fastiggi, Seena Fazel, Duncan S. Ferguson, Helwar Figueroa, Paul Corby Finney, Kyriaki Karidoyanes FitzGerald, Thomas E. FitzGerald, John R. Fitzmier, Marie Therese Flanagan, Sabina Flanagan, Claude Flipo, Ronald B. Flowers, Carole Fontaine, David Ford, Mary Ford, Stephanie A. Ford, Jim Forest, William Franke, Robert M. Franklin, Ruth Franzén, Edward H. Friedman, Samuel Frouisou, Lorelei F. Fuchs, Jojo M. Fung, Inger Furseth, Richard R. Gaillardetz, Brandon Gallaher, China Galland, Mark Galli, Ismael García, Tharscisse Gatwa, Jean-Marie Gaudeul, Luis María Gavilanes del Castillo, Pavel L. Gavrilyuk, Volney P. Gay, Metropolitan Athanasios Geevargis, Kondothra M. George, Mary Gerhart, Simon Gikandi, Maurice Gilbert, Michael J. Gillgannon, Verónica Giménez Beliveau, Terryl Givens, Beth Glazier-McDonald, Philip Gleason, Menghun Goh, Brian Golding, Bishop Hilario M. Gomez, Michelle A. Gonzalez, Donald K. Gorrell, Roy Gottfried, Tamara Grdzelidze, Joel B. Green, Niels Henrik Gregersen, Cristina Grenholm, Herbert Griffiths, Eric W. Gritsch, Erich S. Gruen, Christoffer H. Grundmann, Paul H. Gundani, Jon P. Gunnemann, Petre Guran, Vidar L. Haanes, Jeremiah M. Hackett, Getatchew Haile, Douglas John Hall, Nicholas Hammond, Daphne Hampson, Jehu J. Hanciles, Barry Hankins, Jennifer Haraguchi, Stanley S. Harakas, Anthony John Harding, Conrad L. Harkins, J. William Harmless, Marjory Harper, Amir Harrak, Joel F. Harrington, Mark W. Harris, Susan Ashbrook Harvey, Van A. Harvey, R. Chris Hassel, Jione Havea, Daniel Hawk, Diana L. Hayes, Leslie Hayes, Priscilla Hayner, S. Mark Heim, Simo Heininen, Richard P. Heitzenrater, Eila Helander, David Hempton, Scott H. Hendrix, Jan-Olav Henriksen, Gina Hens-Piazza, Carter Heyward, Nicholas J. Higham, David Hilliard, Norman A. Hjelm, Peter C. Hodgson, Arthur Holder, M. Jan Holton, Dwight N. Hopkins, Ronnie Po-chia Hsia, Po-Ho Huang, James Hudnut-Beumler, Jennifer S. Hughes, Leonard M. Hummel, Mary E. Hunt, Laennec Hurbon, Mark Hutchinson, Susan E. Hylen, Mary Beth Ingham, H. Larry Ingle, Dale T. Irvin, Jon Isaak, Paul John Isaak, Ada María Isasi-Díaz, Hans Raun Iversen, Margaret C. Jacob, Arthur James, Maria Jansdotter-Samuelsson, David Jasper, Werner G. Jeanrond, Renée Jeffery, David Lyle Jeffrey, Theodore W. Jennings, David H. Jensen, Robin Margaret Jensen, David Jobling, Dale A. Johnson, Elizabeth A. Johnson, Maxwell E. Johnson, Sarah Johnson, Mark D. Johnston, F. Stanley Jones, James William Jones, John R. Jones, Alissa Jones Nelson, Inge Jonsson, Jan Joosten, Elizabeth Judd, Mulambya Peggy Kabonde, Robert Kaggwa, Sylvester Kahakwa, Isaac Kalimi, Ogbu U. Kalu, Eunice Kamaara, Wayne C. Kannaday, Musimbi Kanyoro, Veli-Matti Kärkkäinen, Frank Kaufmann, Léon Nguapitshi Kayongo, Richard Kearney, Alice A. Keefe, Ralph Keen, Catherine Keller, Anthony J. Kelly, Karen Kennelly, Kathi Lynn Kern, Fergus Kerr, Edward Kessler, George Kilcourse, Heup Young Kim, Kim Sung-Hae, Kim Yong-Bock, Kim Yung Suk, Richard King, Thomas M. King, Robert M. Kingdon, Ross Kinsler, Hans G. Kippenberg, Cheryl A. Kirk-Duggan, Clifton Kirkpatrick, Leonid Kishkovsky, Nadieszda Kizenko, Jeffrey Klaiber, Hans-Josef Klauck, Sidney Knight, Samuel Kobia, Robert Kolb, Karla Ann Koll, Heikki Kotila, Donald Kraybill, Philip D. W. Krey, Yves Krumenacker, Jeffrey Kah-Jin Kuan, Simanga R. Kumalo, Peter Kuzmic, Simon Shui-Man Kwan, Kwok Pui-lan, André LaCocque, Stephen E. Lahey, John Tsz Pang Lai, Emiel Lamberts, Armando Lampe, Craig Lampe, Beverly J. Lanzetta, Eve LaPlante, Lizette Larson-Miller, Ariel Bybee Laughton, Leonard Lawlor, Bentley Layton, Robin A. Leaver, Karen Lebacqz, Archie Chi Chung Lee, Marilyn J. Legge, Hervé LeGrand, D. L. LeMahieu, Raymond Lemieux, Bill J. Leonard, Ellen M. Leonard, Outi Leppä, Jean Lesaulnier, Nantawan Boonprasat Lewis, Henrietta Leyser, Alexei Lidov, Bernard Lightman, Paul Chang-Ha Lim, Carter Lindberg, Mark R. Lindsay, James R. Linville, James C. Livingston, Ann Loades, David Loades, Jean-Claude Loba-Mkole, Lo Lung Kwong, Wati Longchar, Eleazar López, David W. Lotz, Andrew Louth, Robin W. Lovin, William Luis, Frank D. Macchia, Diarmaid N. J. MacCulloch, Kirk R. MacGregor, Marjory A. MacLean, Donald MacLeod, Tomas S. Maddela, Inge Mager, Laurenti Magesa, David G. Maillu, Fortunato Mallimaci, Philip Mamalakis, Kä Mana, Ukachukwu Chris Manus, Herbert Robinson Marbury, Reuel Norman Marigza, Jacqueline Mariña, Antti Marjanen, Luiz C. L. Marques, Madipoane Masenya (ngwan'a Mphahlele), Caleb J. D. Maskell, Steve Mason, Thomas Massaro, Fernando Matamoros Ponce, András Máté-Tóth, Odair Pedroso Mateus, Dinis Matsolo, Fumitaka Matsuoka, John D'Arcy May, Yelena Mazour-Matusevich, Theodore Mbazumutima, John S. McClure, Christian McConnell, Lee Martin McDonald, Gary B. McGee, Thomas McGowan, Alister E. McGrath, Richard J. McGregor, John A. McGuckin, Maud Burnett McInerney, Elsie Anne McKee, Mary B. McKinley, James F. McMillan, Ernan McMullin, Kathleen E. McVey, M. Douglas Meeks, Monica Jyotsna Melanchthon, Ilie Melniciuc-Puica, Everett Mendoza, Raymond A. Mentzer, William W. Menzies, Ina Merdjanova, Franziska Metzger, Constant J. Mews, Marvin Meyer, Carol Meyers, Vasile Mihoc, Gunner Bjerg Mikkelsen, Maria Inêz de Castro Millen, Clyde Lee Miller, Bonnie J. Miller-McLemore, Alexander Mirkovic, Paul Misner, Nozomu Miyahira, R. W. L. Moberly, Gerald Moede, Aloo Osotsi Mojola, Sunanda Mongia, Rebeca Montemayor, James Moore, Roger E. Moore, Craig E. Morrison O.Carm, Jeffry H. Morrison, Keith Morrison, Wilson J. Moses, Tefetso Henry Mothibe, Mokgethi Motlhabi, Fulata Moyo, Henry Mugabe, Jesse Ndwiga Kanyua Mugambi, Peggy Mulambya-Kabonde, Robert Bruce Mullin, Pamela Mullins Reaves, Saskia Murk Jansen, Heleen L. Murre-Van den Berg, Augustine Musopole, Isaac M. T. Mwase, Philomena Mwaura, Cecilia Nahnfeldt, Anne Nasimiyu Wasike, Carmiña Navia Velasco, Thulani Ndlazi, Alexander Negrov, James B. Nelson, David G. Newcombe, Carol Newsom, Helen J. Nicholson, George W. E. Nickelsburg, Tatyana Nikolskaya, Damayanthi M. A. Niles, Bertil Nilsson, Nyambura Njoroge, Fidelis Nkomazana, Mary Beth Norton, Christian Nottmeier, Sonene Nyawo, Anthère Nzabatsinda, Edward T. Oakes, Gerald O'Collins, Daniel O'Connell, David W. Odell-Scott, Mercy Amba Oduyoye, Kathleen O'Grady, Oyeronke Olajubu, Thomas O'Loughlin, Dennis T. Olson, J. Steven O'Malley, Cephas N. Omenyo, Muriel Orevillo-Montenegro, César Augusto Ornellas Ramos, Agbonkhianmeghe E. Orobator, Kenan B. Osborne, Carolyn Osiek, Javier Otaola Montagne, Douglas F. Ottati, Anna May Say Pa, Irina Paert, Jerry G. Pankhurst, Aristotle Papanikolaou, Samuele F. Pardini, Stefano Parenti, Peter Paris, Sung Bae Park, Cristián G. Parker, Raquel Pastor, Joseph Pathrapankal, Daniel Patte, W. Brown Patterson, Clive Pearson, Keith F. Pecklers, Nancy Cardoso Pereira, David Horace Perkins, Pheme Perkins, Edward N. Peters, Rebecca Todd Peters, Bishop Yeznik Petrossian, Raymond Pfister, Peter C. Phan, Isabel Apawo Phiri, William S. F. Pickering, Derrick G. Pitard, William Elvis Plata, Zlatko Plese, John Plummer, James Newton Poling, Ronald Popivchak, Andrew Porter, Ute Possekel, James M. Powell, Enos Das Pradhan, Devadasan Premnath, Jaime Adrían Prieto Valladares, Anne Primavesi, Randall Prior, María Alicia Puente Lutteroth, Eduardo Guzmão Quadros, Albert Rabil, Laurent William Ramambason, Apolonio M. Ranche, Vololona Randriamanantena Andriamitandrina, Lawrence R. Rast, Paul L. Redditt, Adele Reinhartz, Rolf Rendtorff, Pål Repstad, James N. Rhodes, John K. Riches, Joerg Rieger, Sharon H. Ringe, Sandra Rios, Tyler Roberts, David M. Robinson, James M. Robinson, Joanne Maguire Robinson, Richard A. H. Robinson, Roy R. Robson, Jack B. Rogers, Maria Roginska, Sidney Rooy, Rev. Garnett Roper, Maria José Fontelas Rosado-Nunes, Andrew C. Ross, Stefan Rossbach, François Rossier, John D. Roth, John K. Roth, Phillip Rothwell, Richard E. Rubenstein, Rosemary Radford Ruether, Markku Ruotsila, John E. Rybolt, Risto Saarinen, John Saillant, Juan Sanchez, Wagner Lopes Sanchez, Hugo N. Santos, Gerhard Sauter, Gloria L. Schaab, Sandra M. Schneiders, Quentin J. Schultze, Fernando F. Segovia, Turid Karlsen Seim, Carsten Selch Jensen, Alan P. F. Sell, Frank C. Senn, Kent Davis Sensenig, Damían Setton, Bal Krishna Sharma, Carolyn J. Sharp, Thomas Sheehan, N. Gerald Shenk, Christian Sheppard, Charles Sherlock, Tabona Shoko, Walter B. Shurden, Marguerite Shuster, B. Mark Sietsema, Batara Sihombing, Neil Silberman, Clodomiro Siller, Samuel Silva-Gotay, Heikki Silvet, John K. Simmons, Hagith Sivan, James C. Skedros, Abraham Smith, Ashley A. Smith, Ted A. Smith, Daud Soesilo, Pia Søltoft, Choan-Seng (C. S.) Song, Kathryn Spink, Bryan Spinks, Eric O. Springsted, Nicolas Standaert, Brian Stanley, Glen H. Stassen, Karel Steenbrink, Stephen J. Stein, Andrea Sterk, Gregory E. Sterling, Columba Stewart, Jacques Stewart, Robert B. Stewart, Cynthia Stokes Brown, Ken Stone, Anne Stott, Elizabeth Stuart, Monya Stubbs, Marjorie Hewitt Suchocki, David Kwang-sun Suh, Scott W. Sunquist, Keith Suter, Douglas Sweeney, Charles H. Talbert, Shawqi N. Talia, Elsa Tamez, Joseph B. Tamney, Jonathan Y. Tan, Yak-Hwee Tan, Kathryn Tanner, Feiya Tao, Elizabeth S. Tapia, Aquiline Tarimo, Claire Taylor, Mark Lewis Taylor, Bishop Abba Samuel Wolde Tekestebirhan, Eugene TeSelle, M. Thomas Thangaraj, David R. Thomas, Andrew Thornley, Scott Thumma, Marcelo Timotheo da Costa, George E. “Tink” Tinker, Ola Tjørhom, Karen Jo Torjesen, Iain R. Torrance, Fernando Torres-Londoño, Archbishop Demetrios [Trakatellis], Marit Trelstad, Christine Trevett, Phyllis Trible, Johannes Tromp, Paul Turner, Robert G. Tuttle, Archbishop Desmond Tutu, Peter Tyler, Anders Tyrberg, Justin Ukpong, Javier Ulloa, Camillus Umoh, Kristi Upson-Saia, Martina Urban, Monica Uribe, Elochukwu Eugene Uzukwu, Richard Vaggione, Gabriel Vahanian, Paul Valliere, T. J. Van Bavel, Steven Vanderputten, Peter Van der Veer, Huub Van de Sandt, Louis Van Tongeren, Luke A. Veronis, Noel Villalba, Ramón Vinke, Tim Vivian, David Voas, Elena Volkova, Katharina von Kellenbach, Elina Vuola, Timothy Wadkins, Elaine M. Wainwright, Randi Jones Walker, Dewey D. Wallace, Jerry Walls, Michael J. Walsh, Philip Walters, Janet Walton, Jonathan L. Walton, Wang Xiaochao, Patricia A. Ward, David Harrington Watt, Herold D. Weiss, Laurence L. Welborn, Sharon D. Welch, Timothy Wengert, Traci C. West, Merold Westphal, David Wetherell, Barbara Wheeler, Carolinne White, Jean-Paul Wiest, Frans Wijsen, Terry L. Wilder, Felix Wilfred, Rebecca Wilkin, Daniel H. Williams, D. Newell Williams, Michael A. Williams, Vincent L. Wimbush, Gabriele Winkler, Anders Winroth, Lauri Emílio Wirth, James A. Wiseman, Ebba Witt-Brattström, Teofil Wojciechowski, John Wolffe, Kenman L. Wong, Wong Wai Ching, Linda Woodhead, Wendy M. Wright, Rose Wu, Keith E. Yandell, Gale A. Yee, Viktor Yelensky, Yeo Khiok-Khng, Gustav K. K. Yeung, Angela Yiu, Amos Yong, Yong Ting Jin, You Bin, Youhanna Nessim Youssef, Eliana Yunes, Robert Michael Zaller, Valarie H. Ziegler, Barbara Brown Zikmund, Joyce Ann Zimmerman, Aurora Zlotnik, Zhuo Xinping
- Edited by Daniel Patte, Vanderbilt University, Tennessee
-
- Book:
- The Cambridge Dictionary of Christianity
- Published online:
- 05 August 2012
- Print publication:
- 20 September 2010, pp xi-xliv
-
- Chapter
- Export citation
Contributors
-
- By Claude Alain, Amy F. T. Arnsten, Lars Bäckman, Malcolm A. Binns, Sandra E. Black, S. Thomas Carmichael, Keith D. Cicerone, Maurizio Corbetta, Bruce Crosson, Jeffrey L. Cummings, Deirdre R. Dawson, Michael deRiesthal, Roger A. Dixon, Laura Eggermont, Kirk I. Erickson, Anthony Feinstein, Susan M. Fitzpatrick, Fu Qiang Gao, Douglas D. Garrett, Omar Ghaffar, Robbin Gibb, Elizabeth L. Glisky, Martha L. Glisky, Leslie J. Gonzalez Rothi, Cheryl L. Grady, Carol Greenwood, Gerri Hanten, Richard G. Hunter, Masud Husain, Narinder Kapur, Bryan Kolb, Arthur F. Kramer, Susan A. Leon, Harvey S. Levin, Brian Levine, Nadina Lincoln, Thomas W. McAllister, Edward McAuley, Bruce S. McEwen, David M. Morris, Stephen E. Nadeau, Roshan das Nair, Matthew Parrott, Jennie Ponsford, George P. Prigatano, Joel Ramirez, John M. Ringman, Ian H. Robertson, Amy D. Rodriguez, John C. Rosenbek, Bernhard Ross, Erik Scherder, Victoria Singh-Curry, Trudi Stickland, Donald T. Stuss, Edward Taub, Gary R. Turner, Harry V. Vinters, Samuel Weiss, John Whyte, Barbara A. Wilson, Gordon Winocur, J. Martin Wojtowicz
- Edited by Donald T. Stuss, University of Toronto, Gordon Winocur, University of Toronto, Ian H. Robertson, Trinity College, Dublin
-
- Book:
- Cognitive Neurorehabilitation
- Published online:
- 05 September 2015
- Print publication:
- 11 September 2008, pp ix-xiv
-
- Chapter
- Export citation
Some aspects of interrelations between fungi and other biota in forest soil
- Vladimir KRIVTSOV, Bryan S. GRIFFITHS, Ross SALMOND, Keith LIDDELL, Adam GARSIDE, Tanya BEZGINOVA, Jacqueline A. THOMPSON, Harry J. STAINES, Roy WATLING, John W. PALFREYMAN
-
- Journal:
- Mycological Research / Volume 108 / Issue 8 / August 2004
- Published online by Cambridge University Press:
- 13 August 2004, pp. 933-946
- Print publication:
- August 2004
-
- Article
- Export citation
-
Interrelations of fungal mycelium with other soil biota are of paramount importance in forestry and soil ecology. Here we present the results of statistical analysis of a comprehensive data set collected in the first (and the only) British fungus sanctuary over a period of four months. The variables studied included a number of soil properties, bacteria, protozoan flagellates, ciliates and amoebae, microbial and plant feeding nematodes, various microarthropods, and two fungal biomarkers – glomalin and ergosterol. One way ANOVA showed that the dynamics of the microbiota studied was influenced by seasonal changes. Superimposed on these changes, however, was variability due to biological interactions and habitat characteristics. Two fungal biomarkers, ergosterol and glomalin, were differently influenced by other biota and abiotic variables. The results indicate that the dynamics of soil fungi is influenced not only by soil microarthropods, but also by those found in forest litter. The overall outcome, therefore, is likely to be very complex and will depend upon specific conditions of any particular ecosystem.










